The National Health Insurance Authority has disbursed more than GH¢392 million in vetted claims to healthcare providers across the country, reinforcing efforts to ensure uninterrupted service delivery under the National Health Insurance Scheme.
The payments, made between December 2025 and January 2026, form part of the Authority’s commitment to timely reimbursement of service providers and the financial sustainability of the national health insurance system.
According to official figures released by the Finance Directorate of the Authority, a total of GH¢392,031,851.26 was paid to health facilities for services rendered to NHIS members.
The claims covered submissions made in the previous year and were paid after undergoing the standard vetting and validation processes required under the Scheme. The bulk of the reimbursements was made in December 2025, when the NHIA paid GH¢301,658,338.13 to service providers nationwide.
This was followed by an additional payment of GH¢90,373,513.13 in January 2026. Combined, the two tranches brought total disbursements for the period to just under GH¢400 million, one of the most significant short-term payment cycles recorded by the Authority in recent months.

Officials say the scale of the payments reflects deliberate efforts to reduce outstanding claims and address liquidity challenges faced by healthcare providers.
By clearing a substantial portion of vetted claims, the Authority aims to enable facilities to procure medicines, maintain equipment, and meet operational costs without disruptions that could affect patient care.
Distribution Across Health Facilities
Data from the NHIA show that public and private health facilities together received more than four fifths of the total amount paid during the two month period.
In percentage terms, these facilities accounted for approximately 80.55 percent of all claims settled, highlighting their central role in the delivery of NHIS services nationwide.
In nominal terms, public health facilities received GH¢157,164,301.62, while private health facilities were paid GH¢158,630,317.29. Mission health facilities received the remaining GH¢76,237,232.35, representing 19.45 percent of the total claims paid.
The distribution reflects the diverse mix of providers accredited under the NHIS, spanning government hospitals, private clinics, and faith based health institutions.
The Authority noted that ensuring equitable and timely payments across these categories is essential for maintaining nationwide access to healthcare, particularly in underserved and rural communities where mission and public facilities often serve as the primary points of care.
The NHIA said the payments demonstrate its resolve to promptly reimburse claims so that providers can continue delivering quality services to insured members.
Delays in reimbursement have historically been a major concern for healthcare providers, often affecting cash flow and, in some cases, leading to the rationing of services or delays in treatment.

By accelerating payments, the Authority hopes to strengthen trust between the NHIA and service providers, improve compliance with NHIS protocols, and ultimately enhance patient experience.
Officials emphasised that prompt reimbursement is not only a financial obligation but also a critical component of healthcare quality and system resilience.
NHIS and Financial Sustainability
The latest disbursements come at a time when the NHIS continues to play a central role in Ghana’s healthcare system, providing coverage for a wide range of outpatient and inpatient services.
Ensuring the financial sustainability of the Scheme remains a key policy priority, especially amid rising healthcare costs and growing demand for services. NHIA officials have reiterated that claims payments are subject to rigorous vetting to prevent fraud and ensure value for money.
The Authority has invested in improved claims management systems and periodic audits to strengthen accountability and efficiency in reimbursements.
While acknowledging ongoing challenges, including increasing claims volumes and pressures on funding sources, the NHIA maintains that consistent payments are essential to safeguarding the Scheme’s credibility and long term viability.
Healthcare providers have long argued that timely claims payments directly affect their ability to deliver care. With improved cash flow, facilities are better positioned to stock essential medicines, retain health workers, and maintain infrastructure.
For patients, this translates into fewer service interruptions and greater confidence in the NHIS as a reliable mechanism for accessing healthcare. The sustained reimbursement efforts could also encourage more private providers to remain within the NHIS network, expanding choice and reducing pressure on public facilities.
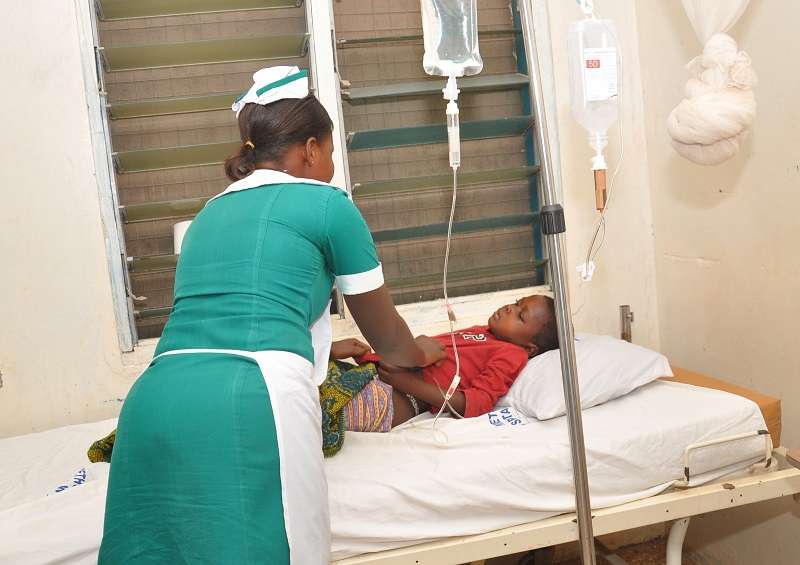
Mission health facilities, which play a critical role in remote and hard-to-reach areas, are also expected to benefit from improved financial stability following the payments.
The NHIA has indicated that it will continue to prioritise the settlement of vetted claims as part of broader reforms aimed at strengthening the NHIS. Future efforts are expected to focus on further reducing claims processing times, enhancing digital systems, and working closely with providers to address operational bottlenecks.
As the Authority moves into 2026, stakeholders will be watching closely to see whether the momentum in claims payments is sustained. For now, the nearly GH¢400 million disbursed over December and January sends a strong signal of intent to support healthcare providers and protect access to care for millions of NHIS members across Ghana.
READ ALSO: Global Electric Car Sales Fall 3% Amid Subsidy Cuts